You are two weeks post-surgery and the compression bra is driving you crazy. The elastic digs into your incision line every time you reach for something. You slept in it last night and woke up itchy and overheated. You are starting to wonder whether this thing is actually helping or just making recovery harder.
Here is what your surgeon’s discharge sheet probably did not cover: the compression bra you were sent home with may not be the right bra for where you are in recovery right now. Swelling shifts. Drains come out. Tissue settles. The bra that fit at discharge often needs adjustment or replacement by week three.
At Front Room Underfashions, our ABC-accredited certified fitters work with women before, during, and after breast surgery. We see what happens when the compression bra fits well and what happens when it does not.
Why Compression Matters After Breast Surgery
A post surgical compression bra is a medical garment that does specific work during the weeks your body is healing.
After any breast surgery, your body responds with inflammation. Blood and lymphatic fluid rush to the surgical site. Without external compression, that fluid accumulates unevenly, which can lead to prolonged swelling, seromas (pockets of fluid under the skin), and complications that may require additional procedures.
Medical-grade compression provides consistent, distributed pressure across the surgical area. It reduces swelling by preventing fluid from pooling. It supports tissue positioning so healing follows the contours your surgeon intended. And it minimizes movement, which reduces strain on internal sutures and incision lines.
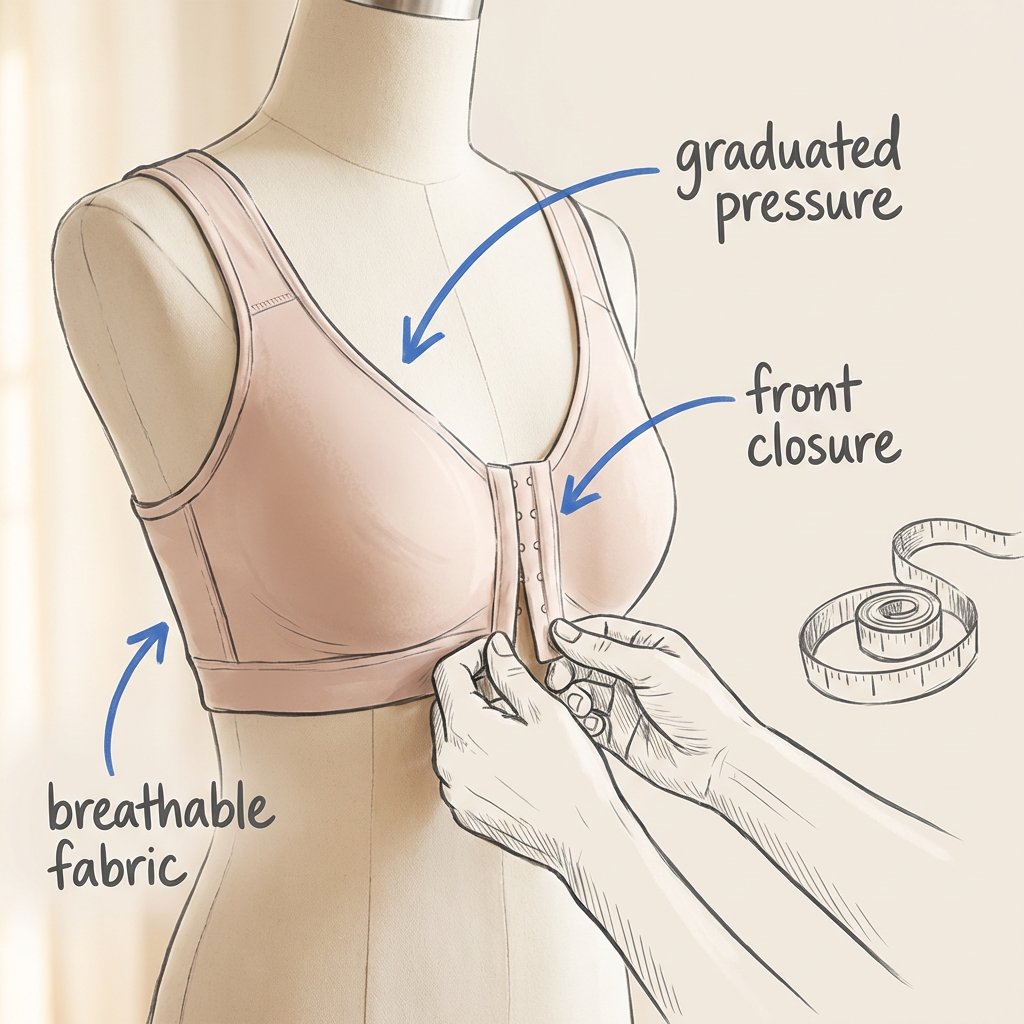
The difference between a well-fitted compression garment and a generic sports bra is significant. A post surgical compression bra applies graduated pressure: firmer at the base where fluid tends to settle, lighter across the upper chest where breathing needs to remain unrestricted. A bra that is too tight in the wrong places can cause as many problems as no compression at all.
Surgery-Specific Timelines
Every surgeon has their own protocol, and you should always follow your surgeon’s guidance first. That said, here is what we consistently see across the hundreds of post-surgical fittings we do each year.
Mastectomy (with or without reconstruction)
Typical compression period: 4 to 8 weeks, sometimes longer with tissue expander reconstruction.
Mastectomy patients often start with a front-closure surgical bra immediately after surgery. If drains are placed, the bra needs built-in drain pockets or enough room for external drain pouches without creating pressure points. Most women transition out of 24/7 wear around week 6. Those undergoing staged reconstruction with tissue expanders may need compression support for several months as the expander gradually stretches the skin.
Breast reduction
Typical compression period: 4 to 6 weeks full-time, then 2 to 4 weeks daytime-only.
Reduction patients carry the most dramatic swelling changes. At discharge, the breasts are often one to two cup sizes larger than the final result. The bra that fits at week one will likely be too loose by week four. We recommend a fitting check at the 3-week mark for reduction patients because the fit shift is almost guaranteed.
Breast augmentation
Typical compression period: 2 to 4 weeks full-time, sometimes with a compression band across the upper pole.
Augmentation recovery tends to be shorter, but implant positioning is critical during the early weeks. Some surgeons prescribe a compression band across the top of the breasts to encourage implants to settle. The bra needs to support from below without pushing upward. If you are wondering what comes after the compression phase, our guide on choosing a bra after breast augmentation walks through the transition in detail.
Breast reconstruction (flap procedures)
Typical compression period: 6 to 8 weeks, with attention to both the breast site and the donor site.
Flap reconstruction creates two surgical sites, and compression garments like the Caromed compression garment address both. These fittings are the most complex because we are balancing support across multiple healing areas.
What to Look for in a Post Surgical Compression Bra
Not every compression bra is built for surgical recovery. Here is what actually matters based on what we see in the fitting room every week.
Front closure. You cannot raise your arms overhead to pull on a bra in the first several weeks. Front-closure designs with hooks, snaps, or adjustable velcro let you dress without straining your incisions.
Adjustable compression. Your body changes week to week. A bra with fixed compression fits one way only. Medical-grade surgical bras with adjustable velcro panels let you increase or decrease compression as swelling changes, extending one bra across your entire recovery.
Drain accommodation. Look for built-in drain pockets or a design that lets drain bulbs sit comfortably without pressing into your body. Pinning drains to the outside of a bra with safety pins creates uneven pressure and risks snagging.
Breathable fabric. You will be wearing this bra 24 hours a day for weeks. Cotton blends and moisture-wicking synthetics reduce the heat and itching. Avoid heavy padding or layered fabrics that trap heat against healing skin.
Wide straps placed away from incision lines. Thin straps concentrate pressure into narrow bands, which is painful over swollen tissue. Wide straps distribute weight more evenly, and for mastectomy patients, strap placement should avoid incision lines and drain sites.
Week-by-Week Fit Changes
This is the part that gets missed, because surgeons do not fit bras. Here is what actually happens to the fit of your compression bra during recovery.
Week 1 brings maximum swelling and minimal movement. The bra should feel snug but not painful. If you cannot take a full breath, it is too tight. Drains are usually still in place, so the bra needs to accommodate them without shifting.
Weeks 2-3 are when most women first notice the bra fitting differently. Swelling begins migrating, often downward and to the sides. The bra may feel looser across the top but tighter at the base. If your bra has velcro panels, this is when you will start adjusting them.
Weeks 4-5 bring significant volume change. Most acute swelling has resolved. Many women find their original compression bra is now too large: the band rides up, the cups gap, and the compression is no longer effective. This is the fitting appointment we recommend most strongly.
Weeks 6-8 are the transition window. If your surgeon clears you to step down from 24/7 compression, start by removing the bra for a few hours during the day, then progress to daytime-only wear, then phase it out. Going straight from full compression to a regular bra often results in increased swelling that sends women right back.
Solving Common Comfort Complaints
Itching under the band is usually caused by heat, moisture, or friction. A thin cotton liner between the bra and your skin helps immediately. Wash the bra every two to three days with fragrance-free detergent. For related skin concerns during recovery, our guide to managing dry skin after breast surgery covers what to use and what to avoid.
Sleeping discomfort is real, but a small pillow under each arm reduces pressure on the sides. Sleep on your back with your upper body slightly elevated. If the front closure hardware digs into your sternum, a thin piece of moleskin over the closure point helps.
Shoulder and neck strain usually means the bra is doing too much work from the straps and not enough from the band. A properly fitted compression bra gets 80 percent of its support from the band. If your straps leave red marks, the band is too loose or has stretched out.
Transitioning Out of Compression
The move from surgical compression to an everyday bra should happen gradually over one to three weeks. Here is how to do it without setbacks.
Signs you are ready: Your surgeon has given clearance. Swelling has been stable for at least a week. You can go several hours without the bra and notice no increased swelling. Incision lines are fully closed and no longer tender.
The gradual approach: Start by removing the compression bra for 2 to 3 hours while resting at home. Extend to half the day while keeping compression at night and during activity. Switch to a soft, wireless, front-closure bra during the day. Then phase out nighttime compression over another week.
Your first bra after compression should be wireless, soft-cup, and front-closure. Underwire creates pressure points that can interfere with tissue settling, especially after augmentation or reconstruction. If you are preparing for your first post-mastectomy bra, a fitting at the transition point ensures the bra fits the body you have now, not the body you had before surgery.
Your Recovery Deserves a Bra That Fits Every Stage
Front Room Underfashions is an ABC-accredited post-surgical fitting boutique with nearly 40 years of experience. Our certified fitters work with women before surgery so your compression garment is ready at discharge, and through every phase of recovery after.
If you are preparing for breast surgery or struggling with your current compression bra, schedule a fitting consultation. We will check where you are in recovery, assess your current fit, and make sure your compression bra is actually doing what it needs to do.
Frequently Asked Questions
How long should you wear a compression bra after breast surgery?
Most surgeons recommend 4 to 8 weeks of full-time wear, depending on surgery type. Mastectomy: 4 to 8 weeks. Reduction: 4 to 6 weeks full-time plus 2 to 4 weeks daytime-only. Augmentation: 2 to 4 weeks. Always follow your surgeon’s guidance and have your fit checked at weeks 3 and 6.
Can you sleep in a compression bra after surgery?
Yes, and you should during the first several weeks. Sleep on your back with your upper body elevated and a pillow under each arm. Most women phase out nighttime compression before daytime compression during the transition period.
How tight should a post surgical compression bra be?
Snug and supportive, but you should be able to take a full breath. If you cannot breathe deeply, it is too tight. If you can fit more than two fingers under the band, it may be too loose. Swelling changes will alter the fit week to week.
When can I switch to a regular bra after surgery?
Most women begin transitioning between weeks 6 and 8 after surgeon clearance. Transition gradually over 1 to 3 weeks. Your first regular bra should be wireless, soft-cup, and front-closure. Avoid underwire for at least 3 months after surgery.
Does insurance cover post surgical compression bras?
Many plans cover compression garments when prescribed by your surgeon, particularly after mastectomy under the Women’s Health and Cancer Rights Act. Ask your surgeon for a prescription before your procedure. Our staff can help you understand your coverage options.